Yet despite the clarity of medical reports and the unanimous assessments from specialists, subtle observations in the hours leading up to a pivotal moment—small, almost imperceptible responses—were quietly noted by staff but not fully documented, leaving lingering questions about whether the situation had always been as irreversible as initially concluded.
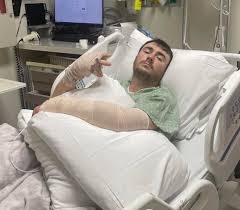
In the highly controlled environment of a Houston intensive care unit, every monitor reading carries weight. Medical teams rely on neurological scans, vascular evaluations, and continuous vital signs to guide decisions. These tools are designed to provide objective clarity, minimizing ambiguity.
For weeks, these very measurements had painted a discouraging picture for Hunter Alexander: the nerve damage affecting his upper extremities was deemed permanent.
Specialists from across the country—vascular surgeons and neurologists alike—had reviewed his case. Their consensus was firm: given the severity of his injuries, the multiple surgeries he had undergone, and the complications following a catastrophic arterial rupture, recovery of hand function was considered highly unlikely. The word “permanent” reflected a carefully weighed conclusion, grounded in clinical evidence and repeated evaluations.
Hunter’s condition resulted from a complex medical crisis requiring five separate surgeries, each aimed at stabilizing his health and preventing further deterioration. The cumulative effects of trauma, combined with the delicate process of nerve regeneration, led physicians to conclude that the pathways responsible for movement and sensation in his hands had been irreparably damaged.
For his family—particularly his mother, Katie—the experience became an extended vigil. Day after day, she remained by his bedside in Room 302, measuring time not in hours but in progress—or the absence of it.
The environment was dominated by the hum of machines, the rhythmic beeping of monitors, and the quiet efficiency of rotating staff.
By the 168-hour mark, the emotional toll rivaled the physical. Conversations had shifted from recovery possibilities to long-term adaptation strategies. Terms such as “atrophy,” “irreversible damage,” and “nerve degeneration” became part of the family’s daily vocabulary. Doctors delivered these updates with empathy, balancing honesty with sensitivity, gradually moving the outlook from uncertain to guarded, and finally to a consensus that functional recovery was unlikely.
Yet on one evening, a subtle shift occurred. At 8:14 PM, a small but notable response was observed in Hunter—an isolated movement that, in weeks of static readings, stood out. For Katie, who had scrutinized every micro-change, such a moment carried profound significance.
Medical professionals approached the observation cautiously. In intensive care, isolated movements are never immediately interpreted as signs of recovery. They are documented, analyzed, and considered alongside the broader clinical picture. Even so, moments like these often prompt renewed attention and careful reassessment.
Throughout the night, staff continued monitoring Hunter closely, maintaining treatment protocols while watching for any further changes. While the observation did not instantly overturn previous assessments, it added a new layer to an already complex situation.
For the family, the emotional weight of that moment was immediate. After weeks of hearing consistent opinions emphasizing permanence, even a minor sign of change could feel momentous. It did not erase the challenges ahead, but it suggested that the narrative might not be entirely fixed.
As the ICU returned to its steady rhythm, with monitors tracking vital signs and staff attending to their duties, the significance of that evening lingered in Room 302. It became a point of reflection, a subtle reminder that in critical care, medical certainty and human resilience sometimes intersect in unexpected ways.
Conclusion
Hunter Alexander’s case illustrates the delicate balance between clinical certainty and the unpredictable nature of recovery. Early assessments suggested permanent nerve damage, yet the events of that evening introduced a hint—however slight—that the final outcome was not predetermined.
In critical care, such observations are documented with caution, but for families like Katie’s, they carry emotional weight, offering a measure of hope amid uncertainty. Room 302 stands as a testament to both the rigor of medicine and the enduring human desire to witness even the smallest signs of resilience.
